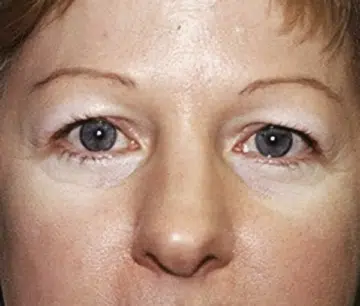
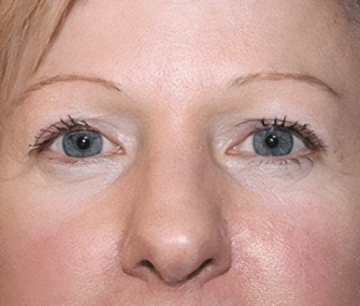
Looking older than you feel?
Book a consultation today to look refreshed and vibrant!
Plastic Surgery in Eau Claire, Wisconsin
Welcome to a New Found Confidence
Looking for some options for cosmetic or reconstructive surgery? Our website, procedures pages, and photo gallery, have a wealth of information available to those looking for procedures anywhere from eyelid surgery, breast augmentation, tummy tuck, breast reconstruction, and mommy makeover. Dr. Ewings offers a diverse skin care line for women named Enza Essentials.
If you have questions please give us a call at 1-800-456-8222 or contact us today!
Dr. Ember Ewings
For over a decade, Dr. Ember Ewings has taken pride in delivering excellence in plastic surgical care. She earned her medical degree from the University of Wisconsin-Madison School of Medicine, and completed her residency training in plastic surgery at Saint Louis University. Additionally, she gained extensive experience in pediatric and craniofacial surgery during her fellowship at the University of Tennessee – Memphis, and Hôpital Necker-Enfants Malades in Paris, France. She is board Certified by the American Board of Plastic Surgery.
Dr. Ewings has enjoyed caring for patients of all ages from across the upper Midwest, and performs both cosmetic surgical, non-surgical, and reconstructive procedures. She is delighted to be able to provide outreach services in Durand, Wisconsin.








What Our Patients Are Saying